Dimethyl Sulfoxide Increases the Survival of Primarily Ischemic Island Skin Flaps
Robert J. Carpenter, MD, Michael F. Angel. MD, and Raymond F. Morgan, MD
Rochester, New York
Summary
There is ample evidence of the involvement of free
radicals in mediating skin flap necrosis. Dimethyl sulfoxide
(DMSO) is a well-tolerated, safe drug that is a powerful
scavenger of the hydroxyl free radical. The current
study investigated the effect of DMSO on the survival
of 9 x 4 cm skin flaps based on the epigastric
vessels subjected to primary venous occlusion. Forty-seven
skin flaps were elevated and the epigastric vein was
occluded by a microvascular clamp for 8 hours. Group
1 received DMSO (1.5nbsp;gm/kg) intraperitoneally at
reperfusion. Group 2 received saline solution,
group 3 received DMSO at reperfusion and every day for
5 days, group 4 received DMSO preoperatively and
then as in group 3, and group 5 was the saline
solution control for groups 3 and 4. DMSO did not
increase percent flap survival when given as a single
dose at reperfusion (40.6% ± 42.7%) compared
with saline solution (33.7% ± 41.2%).
When DMSO was continued in the postoperative period,
group 3 (86.2% ±nbsp;25.8%) and group
4 (78.0% ± 32.5%) had significantly better
survival than the saline solution control group (32.6% ± 39.8%)
(p < 0.01 and p < 0.03, respectively).
There was no significant difference between groups 3
and 4. DMSO administered at reperfusion and postoperatively
for 5 days significantly increased flap survival. It
is hypothesized that this occurs through scavenging
deleterious free radical species. This effect may have
clinical significance. (Otolaryngol Head Neck Surg 1994:110: 228-31.)Increasing interest in the mechanisms of ischemia/reperfusion
injury has been sparked by technical advances in plastic
surgery such as free tissue transfer, limb replantation,
and the use of long vascular pedicles. The production
of oxygen-derived free radicles (OFRs) is widely recognized
as a major cause of reperfusion injury in many organ
systems. 1, 2 Importantly,
survival of both random and axial skin flaps has been
reported to be heavily influenced by OFR production.
3-6 Agents that block the
formation of OFRs (allopurinol,7, 8
soybean trypsin inhibitor9)
as well as OFR scavengers (superoxide dismutase,3
mannitol,8, 9 DMSO,9
desferoxamine,5 and N-2-mercaptopropioniglycine9)
have all been shown to increase survival of skin flaps.Dimethyl sulfoxide (DMSO) was first synthesized in
1866. It has a pyramidal structure, with sulfur at the
center and two methyl groups and an oxygen atom (with
a nonbonding electron pair) at the apices. Because of
this structure, DMSO has exceptional solvent properties.
The free electron pair allows it to participate in the
transfer of electrons and makes DMSO a free radical
scavenger with a high degree of specificity for the
damaging hydroxyl radical. Investigators have found
that DMSO lessens reperfusion injury in a variety of
tissues, including intestine,10, 11
kidneys,12 muscle,13
and skin. 8
Figure
1
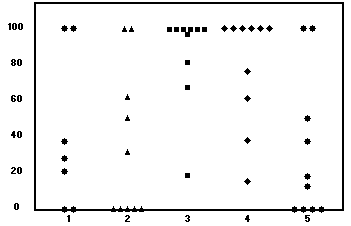
Fig. 1. DMSO study: Percent flap survival. Group 1,
reperfusion; group 2, control; group 3, reperfusion + 5 days; group 4, pretreatment + 5 days; and group 5,
control.
Figure
2
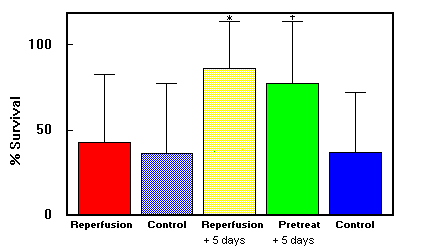
Fig. 2. DMSO study: Mean (±SD) survival in skin
flap groups. *Group 3 had better survival rate
than group 1 (p < 0.01>. tGroup 4
had a better survival rate than group 5 (p < 0.03).Early studies with DMSO demonstrated enhanced survival
in a dorsal flap model,14
which was an an axlal flap with a random extention.
Others have confirmed this finding. 15
Narayanan et al. 9 found that DMSO enhanced flap survival in a different
model. Epigastric island flaps were subjected to 15
hours of total primary ischemia. Skin flap survival
increased from 13% to 63% with the administration of
DMSO.The current study evaluated the effectiveness as well
as optimal timing of administration of DMSO in a model
of primary venous occlusion.
Methods
and Materials
Female Sprague/Dawley rats (n = 47), weighing
230 to 249 gm each, were used. They were housed
individuaIly and given water and rat chow ad Iibitum.
Animals were humanely cared for in compliance with The
Principles of Laboratory Animal Care, formulated
by the National Society for Medical Research, and the
Guide for the Care and Use of Laboratory Animals,
prepared by the National Academy of Sciences and published
by the National Institutes of Health. With the animals
under pentobarbital anesthesia (35 mg/kg intraperitoneally),
a 9 x 4 cm abdominal flap, based on the left
epigastric neurovascular pedicle, was elevated as previously
described by others16 and
resutured to its bed. The medial border of the flap
formed a line runing from xiphoid to pubis. The vein
of the flap was then occluded with a microvascular clamp
for 8 hours. After removal of the clamp, the vein
was observed to assure the return of venous blood flow.
DMSO (Sigma Chemical, St. Louis, Mo.) was given intraperitoneally
(1.5 mg/kg) according to the following protocol:
Group 1 (reperfusion only): DMSO
was given at reanesthesia for removal of the microvascular
clamp on the vein (n = 7)Group 2 (controls for group 1): received 0.2 ml normal saline solution intraperitoneally
as in group 1 (n = 10)Group 3 (reperfusion + 5 days): DMSO was given as in group 1 and then continued
daily for 5 days (n = 10)Group 4 (pretreatment + reperfusion
+ 5 days): DMSO was given before initial flap elevation,
then as in group 3 (n = 10)Group 5 (controls for groups 3 and
4): 0.2 ml normal saline solution was given
on the same schedule as in group 4
Flap viability was assessed on postoperative day 5.
The area of survival was calculated using a sonic digitizer
and expressed as a percent of the original total flap
area as previously described. 17
The Wilcoxon-Mann-Whitney two-sample test and the Kruskal-Wallis
K-sample test were used to determine significance.
Results
Data are summarized in Figs. 1
and 2 and Table 1.
DMSO showed no increase in flap survival when given
as a single intraperitoneal dose at reperfusion (40.6% ± 42.7%)
when compared with saline solution (33.7% ± 41.2%).
Continuing DMSO administration postoperatively increased
the percentage of flap survival significantly (86.3% ± 25.8%)
compared with control (32.6% ± 39.8%; p < 0.01), Pretreatment with DMSO
before the onset of ischemia (78.0% ± 32.5%)
did not confer survival benefit compared with beginning
treatment at reperfusion.
Table
1
| Group
no. |
Average
percent flap survival |
P
value |
| 140.6
± 42.7 |
>
0.05 |
| 233.7
± 41.2 |
NS |
| 386.2
± 25.8 |
0.011 |
| 478.0
± 32.5 |
0.026 |
| 532.6
± 39.8 |
NS |
Discussion
DMSO has been extensively studied by both chemists
and physicians. It is a small (78 molecular weight)
molecule that readily crosses the membranes of cells
and organelles as well as intact skin. DMSO scavenges
the hydroxyl radical (OH), one of the most toxic by-products
of superoxide radical formation. Schlafer18 noted DMSO to be an ideal OH scavenger because it (1) is
specific for OH, (2) reaches the sites of OH generation
(down to the mitochondrial level), and (3) lacks
cellular toxicity.DMSO also causes vasodilation in small and intermediate
vessels, which can be blocked by the administration
of antihistamines. 14, 15DMSO has shown mixed results in increasing skin flap
viability when used topically. 14
However, when administered either intraperitoneally
or intravenously, DMSO increased survival in both random
and island skin flap models. 9,
20, 21The current model is an axial flap with a random extension.
In addition, it received a primary ischemic insult by
venous obstruction as first described by Harashina et
al. 16 In this model,
therefore, several processes are occuring. The distal
part of the flap is in a partially ischemic state, which
is a source of free radical production. 22
Once venous obstruction occurs, further stresses are
placed on the entire flap: hydrostatic forces increase,
and ischemia occurs with production of free radicals
and other mediators of tissue destruction. 23, 24The current study failed to show a benefit when DMSO
was given as a single dose at reperfusion. This is in
contrast to the experience of Narayanan et al.,9
who found significant survival benefit from a single
dose of DMSO. This discrepancy between studies is not
unexpected. The dose of DMSO used in Narayanan et
al.'s work (5 gm/kg) was more than threefold
our dose (1.5 gm/kg). In addition, the experimental
models are different. The former study uses an axial
flap that underwent 15 hours of primary arterial ishemia.
Production of OFRs would be expected to be maximal during
the period of reperfusion. In our study, by contrast,
flaps suffered OFR production throughout the venous
obstruction, reperfusion, and postreperfusion periods.
From this scenario one would expect DMSO to be beneficial
when given at these times of OFR production. Therefore,
group 4, which received DMSO before the reperfusion
and during the postreperfusion period, had significantly
better survival than control animals. In this study,
however, administration of DMSO before venous obstruction
offered no additional benefit. This may be explained
by hypothesizing that although OFRs are produced during
primary venous obstruction, there are other, more important
damaging processes (i.e., hydrostatic forces) that are
unaffected by DMSO.DMSO is a safe, well-tolerated drug. 6,
25 It has demonstrated beneficial
effects in a number of models and organ systems. It
significantly improves flap survival in this study and
may have clinical significance.
References
- Bulkley GB. Pathophysiology of free
radical-mediated reperfusion injury. J Vasc Surg
1987; 5:512.
Angel MF. Ramasastry SS, Swartz WM,
Basford RE, Futrell J. Free radicals: basic concepts
concerning the chemistry, pathophysiology, and relevance
to plastic surgery. Plast Reconstr Surg 1987;
79:990.
Manson PN, Anthenelli RM, lm MJ, Bulkley
GB, Hoopes JE. The role of oxygen-free radicals in
ischemic tissue injury in island skin flaps. Ann
Surg 1983; 1983:87.
Huang L. Privalle CT, Serafin D, Klitzman
B. Increased survival of skin flaps by scavengers
of superoxide radical. FASEB J 1987; 69:469.
Angel MF, Narayanan K, Swartz WM,
et al. Deferoxamine increases skin flap survival:
additional evidence of free radical involvement in
ischemic flap surgery. Br J Plast Surg 1986;
69.469
Kim YS, lm MJ, Hoopes J. The effect
of a free radical scavenger, N-2-Mercaptopropionyiglycine,
on the survival of skin flaps. Ann Plast Surg
1990; 25:15.
IM MJ, Shen W, Pak CJ, Manson PN,
Bulkley GB, Hoopes J. Effect of allolpurinol on the
survival of hyperemic isIand skin flaps. Plast
Reconstr Surg 1984; 73:276.
Angel MF, Narayanan K, Swartz WM,
Ramasastry SS, Basford RE, Futrell J. Augmentation
of skin flap survival with allopurinol. Ann Plast
Surg 1987; 18:494
Narayanan K, lm MJ, Manson PN, Bulkley
GB, Hoopes J. Mechanism and prevention of ischemia/reperfusion
injury in isIand skin flaps. Surg Forum 1985;
36:593.
Parks DA, Shah AK, Granger D. Oxygen
radicas: effects on intestinal vascular permeability.
Am J Physiol 1984; 247:167.
Ravid M, Van-Dyk D, Berneim J. The
protective effect of dimethyl sulfoxide in experimental
ischemia of the intestine. Ann NY Acad Sci
1983; 411:131.
Kedar I, Jacob ET, Bar-Natan N, Ravid
M. DimethyI sulfoxide in acute ischemia of the kidney.
Ann NY Acad Sci 1983; 411:131.
Feller AM, Roth AC, Russell R. Experimental
evaluation of oxygen free radical scavengers in prevention
of reperfusion injury in muscle. Ann Plast Surg
1989; 22:131.
Adamson JE, Hotton CE, Crawford HH,
Ayers W. Studies on the action of dimethyl sulfoxide
on the experimental pedicle flap. Plast Reconstr
Surg 1989; 22:321.
Haller J, Trachy, Cummings R. Effect
of dimethyl sulfoxide on island flap perfusion and
survival in rats. Arch Otolaryngol Head Neck Surg
1987: 113:859.
Harashina T, Sawada Y, Watanabe S.
The relationship between venous occlusion time in
island skin flaps and flap survival. Plast Reconstr
Surg 1977; 60:92.
Nichter LS, Sobieski MW, Morgan RF,
Rodeheaver G, Edlich R. Quantitation of skin flap
survival: a computer based method. Plast Reconstr
Surg 1984; 73:684.
Schlafer M. Cardiac pharmacology
of dimethyl sulfoxide and its postulated relevance
to organ preservation in ischemic or hypoxic states.
Ann NY Acad Sci 1983; 411:170.
Koehnlein HE, Lemperle G. Experimental
studies on the effect of dimethyl sulfoxide on pedicle
flaps. Surgery 1970; 67:672.
Arturson G, Khanna N. The effects
of hyperbaric oxygen, dimethyl sulfoxide, and Complamin
on the survival of experimental skin flaps. Scand
J Plast Reconstr Surg 1970: 4.8.
Grossman JAI, McGonagle BA, Dowden
RV,Dinner M. The effect of hyaluronidase and dimethyI
sulfoxide (DMSO) on experimental skin flap survival.
Ann Plast Surg 1983: 11:223.
Angel MF, Ramasastry SS, Swartz WM,
Narayanan K, Kuhns DB, Futrell J. The critical relationship
between free radicals and degrees of ischemia: evidence
for tissue intolerance of marginal perfusion. Plast
Reconstr Surg 1988; 81:233.
Angel MF, Mellow CJ, Knight KR, Morgan
RF, O'Brien McC. Biochemical analysis of acutely ischemic
skin flaps. Curr Surg 1990: 47:272.
Im MJ, Manson PN, Bulkley GB, Hoopes
J. Effects of superoxide dismatase and allopurinol
on the survival of acute island skin flaps. Ann
Surg 1985; 201:357.
- Trice JM, Pinals RS. Dimethyl sulfoxide:
a review of its use in the rheumatic disorders. Semin
Arthritis Rheum 1985: 15:45.
Source
From the Department of Surgery (Dr. Carpenter). University
of Rochester School of Medicine; the Division of Plastic
Surgery (Dr. Angel), The Johns Hopkins School of Medicine,
and the Department of Plastic Surgery. (Dr. Morgan),
University ofVirginia Health Sciences Center.Received for publication March 12, 1993; revision received
June 9, 1993; accepted June 17, 1993. Reprint requests: Robert J. Carpenter, MD. Department
of Plastic Surgery, The Johns Hopkins Hospital, 601
North Caroline St./McElderry 8152C, Baltimore, MD 21287.
Copyright © by the American Academy of Otoloryngology-Head
and Neck Surgery Foundation, Inc. 0194-5998/94/$3.00 + 0 23/10/49496
DMSO wishes to thank to thank the publishers for their
kind permission to put this document on our web site.
Copyright for this article is retained by the publisher.
Permission to copy any portion of this document must
be obtained from the publisher.
|



